Book Your Free Consultation
Mr David Allamby
MD, FRCOphth, FRCS
BOOK A CONSULTATION
Cataracts make your vision blurry or dim. Cataract surgery restores clear vision by replacing the misty lens inside your eye with a new, clear implant

Cataract surgery is an operation used to treat cataracts that are affecting your daily life. More than 300,000 procedures are carried out each year in the UK, making it the most common operation of any speciality performed in the country.
Cataracts can usually be treated with a routine day case operation where the cloudy lens is removed and is replaced with an artificial plastic lens. Lens surgery is a very established procedure and was first performed in 1950.
Cataract surgery takes 10-15 minutes to complete
Since then the operation has consistently evolved; current techniques using ultrasound and a keyhole approach have demonstrated an excellent safety track record.
A cataract is a clouding of the normally clear lens inside the the front part of eye. It causes a loss of vision that cannot be fixed with glasses or contact lenses. Cataracts are very common, especially among those aged 70+.
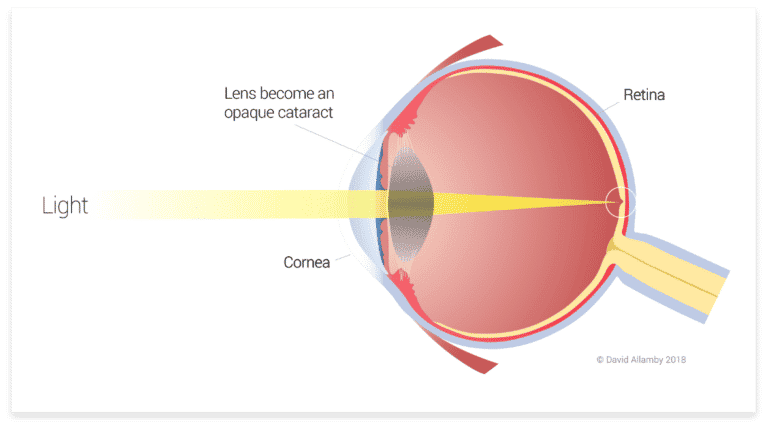
A cataract blocks light from passing through the lens, reducing the brightness and clarity of vision. You can think of a cataract as frosted rather than clear glass; the whitening of frosted glass doesn’t allow a clear image to be seen.
The whitened opacity of a cataract affects sight in the same way, preventing a clear image being made on the retina inside the eye. Laser refractive surgery, such as LASIK, is not effective.
Cataracts are not usually painful and do not usually cause any redness or inflammation. They develop slowly and painlessly over months or years.
You may notice that colours appear faded and that your vision is not as sharp as it used to be. You may also find it more difficult to see at night or in dimly lit conditions. You may even notice a 'halo' around lights.
Cataracts are very common. More than half of all people aged over 65 have some degree of cataract development. By the age of 80, around 80% will have a cataract in at least one eye.
Cataracts can develop over a number of years and may initially cause no symptoms. They usually develop in both eyes, although one eye may be more advanced than the other.
You can think of a cataract as frosted rather than clear glass, preventing clear vision
Your vision can become misty or blurred, or you may have small patches where your vision is fogged, even when wearing your glasses. Common visual symptoms from cataracts include the following:
Cataracts are very treatable and Focus offer modern, minimally invasive surgery. Contact us for more information on our advanced cataract removal procedures.
Precisely why cataracts occur is not known, although they appear to be caused by alterations in proteins within the lens that develop over many years, changing it from clear to cloudy. Cataracts are linked with:
Irrespective of the cause, when cataracts affect vision to the point of interfering with daily activities they are treated by surgical removal. Apart from avoiding removable causes above, there is no known prevention.
Prior to cataract operation, your ophthalmologist will perform a complete eye health examination to check the overall condition of your eyes, determine any risk factors, and exclude any reasons why you should not have surgery.
A measurement of any glasses prescription, called a refraction, will be performed to accurately determine your degree of short-sight, long-sight and any astigmatism you have prior to surgery. Additional measurements include biometry (a detailed ultrasound scan to measure all the anatomical dimension, including the length of your eye) and topography to determine the curvature of your cornea.
Your surgeon needs all these measurements to select the proper power of the intraocular lens implant to give you the most detailed vision possible after the operation.
Your surgeon will also discuss the various types of lens implants available prior to your cataract surgery, as well as describing what to expect before, during and after your procedure.
If you have cataracts in both eyes, your surgeon may treat your right and left eyes on the same day, or may ask that you wait 1 to 3 weeks between procedures. For those patients who are having both eyes treated on the same day, you will typically have a check-up one or two days later. The choice will depend on your prescription and surgeon recommendation.
Cataracts are often detected during an eye examination, either with your local optometrist or an eye doctor. You may or may not have noticed a drop in vision, depending on how far the cataract has progressed. The opacified areas of the lens can be most easily seen using a slit-lamp microscope (a vertical microscope controlled by a joystick, shining a bright slit of light at your eye while your chin sits upon a chin-rest).
Using a variety of tests, a doctor is able to tell how much a cataract may be affecting vision. Usual eye tests include:
A full eye examination will confirm that the loss of sight is not because of other common eye problems, such as diabetes, glaucoma, or age-related macular degeneration (AMD).
Some people worry that they will need to have a cataract operation as soon as they are diagnosed with cataracts. In most cases, however, there is no rush to have surgery as the cataract will grow slowly and your vision will only worsen gradually.
Your optometrist will usually closely monitor your cataracts at regular intervals, typically every 6 to 12 months, and will refer you to an ophthalmic surgeon when they feel the time is right for you to have an operation.
Surgery for cataract is very effective at restoring vision. The misty or opaque cataract needs to be removed and replaced with a new clear implant, known as an intraocular lens (IOL). The procedure takes 10-15 minutes per eye and is typically is performed as a day case, without needing an overnight stay in hospital.
Modern cataract operations include the use of high-frequency ultrasound, known as phacoemulsification, or ‘phaco’
In most cases, treatment will be performed under local anaesthetic (you are awake but the eye is numbed). Modern cataract operations include the use of high-frequency ultrasound, delivered via a special hand-piece, that breaks up the misty lens into very small pieces. These fragments are then gently removed from the eye with minimal suction.
This surgical approach is known as phacoemulsification or “phaco” for short. It can be performed with much smaller incisions than prior techniques for cataract removal, allowing quicker healing and reducing some of the risk of cataract surgery complications, such as retinal detachment.
Once all of the cloudy lens has been removed, your surgeon inserts a clear specially designed implant, called an intraocular lens (IOL), placing it securely in the space created after removal of your natural lens.
The final step is for your surgeon to close the incision in your eye, usually without the need for a stitch. A protective plastic shield protects your eye while it heals in the post-op recovery phase.
Cataract surgery is now a very successful and safe procedure. It is one of the most commonly performed surgical procedures in England, with over 400,000 operations carried out each year.
After the operation, you will be given antibiotic eye drops to help with healing and to prevent infection. Your surgeon will also give you some post-operative advice, which will include:
After a few days, most patients feel comfortable enough to return to their normal activities. It can take up to eight weeks for your vision to fully recover and for you to see as clearly as possible.
You will usually need to have a check-up with your surgeon anywhere between one and four weeks after surgery.
It's normal for your vision to be a little blurry immediately after surgery. This usually improves within a few days or weeks as your eye heals and adjusts to the new lens.
Some people experience what's known as second sight following surgery. This means that, for the first time in years, they can see clearly without glasses or contact lenses.
Itching and a sensation that there's something in your eye are also common after cataract surgery. These symptoms usually resolve within a few weeks as your eye heals.
Most people who have cataract surgery experience a significant improvement in their vision. However, it's not possible to guarantee perfect vision after surgery as the eye is a delicate organ and, like any operation, there's always a small risk of complications.
If you experience any problems after surgery, such as severe pain, new vision problems, or increased redness or swelling in your eye, you should contact your surgeon immediately.
The majority of people who have cataract surgery don't experience any problems. However, as with any type of surgery, there are a number of potential complications that can occur. The most common complication is posterior capsule opacification (PCO), also known as secondary cataract.
This occurs when the back of the lens capsule (the clear membrane that holds the IOL in place) becomes cloudy. PCO is usually treated with a simple laser treatment, which takes just a few minutes to perform.
Other potential complications that can occur after cataract surgery include:
Most of these complications are rare, and can usually be treated with medication or further surgery. In very rare cases, cataract surgery can lead to permanent vision loss.
If you experience any problems after cataract surgery, it's important to see your surgeon as soon as possible so that they can investigate and treat any complications.
Cataract surgery is a very successful operation and most people who have it experience a significant improvement in their vision. In fact, around 98% of people who have cataract surgery don't experience any problems and are satisfied with the results.
Cataract operation can also:
As well as improving your vision, cataract surgery can also help to treat other eye conditions, such as glaucoma and macular degeneration. In some cases, it can even prevent these conditions from developing in the first place.
People who have cataracts are also at a higher risk of developing serious eye conditions. Cataracts can cause the retina to become detached, which can lead to blindness. Other serious conditions that cataracts can cause include glaucoma, eye inflammation, and macular degeneration.
Cataract surgery can help to protect your sight by removing cataracts and preventing these serious conditions from developing.
Cataract surgery can also improve your quality of life. It can help you to stay independent and active, as well as give you the confidence to socialise and enjoy your hobbies. The surgery can also help you to stay employed and earn a higher salary.
Cataracts can also increase your risk of injury. This is because cataracts can make it difficult to see, which can lead to accidents. Imagine trying to drive with cataracts – you would be at a greater risk of having an accident.
Cataract surgery can help to keep you safe from injury by improving your vision and making it easier for you to see.
With private surgery, you have a wide choice for which IOL you would like implanted. Your options though come under three main lens choices, depending if you would like to minimise the need for reading glasses after surgery:
IOLs that correct short-sight and long-sight are standard mono-focal implants, and the type used in the NHS. There are now toric IOLs that correct astigmatism as well.
If you don’t mind wearing glasses after cataract surgery, a monofocal lens implant usually is used. You will need reading glasses after cataract surgery with monofocal IOLs. New glasses can be prescribed for you approximately one month after surgery.
If you like the idea of being less dependent on glasses after cataract surgery, one way to correct presbyopia and reduce your need for reading glasses is to have your cataract surgeon adjust the power of one of your monofocal IOLs (assuming you have cataract surgery performed in both eyes) to give you a monovision correction, similar to monovision with contact lenses.
Another option is to choose one of a variety of advanced presbyopia-correcting IOLs to improve your reading vision without sacrificing your distance vision. Presbyopia-correcting IOLs include bifocal and trifocal IOLs; both types are designed to provide a greater range of vision after cataract surgery than conventional monofocal IOLs.
Be aware that not everyone is a good candidate for these premium IOLs, and choosing a presbyopia-correcting IOL is only available privately.
Cataract surgery is a serious operation, and it is important to choose the right surgeon to perform the surgery. You should look for a surgeon who is experienced and has a good track record.
You should also make sure that you are comfortable with the surgeon and that you feel confident in their ability to perform the surgery.
At Focus clinics, we have a team of experienced and qualified surgeons who can perform cataract surgery. We offer a free consultation so that you can meet with one of our surgeons and discuss your options.
We also offer a wide range of lens implants, so you can choose the right one for your vision. To book a free consultation, fill in our online form or call us on 0207 307 8250. We look forward to helping you improve your vision.
Normally the vision is soft focus immediately after surgery and the next day vision is often good.
Common sense needs to be applied but people can bend over, wash, shop and carry out general activities.
On the day following surgery you can take a bath or shower and use a computer. Sports can be resumed after a few weeks or a month.
Flying as a passenger can be done the day after surgery but as a pilot the necessary licensing needs to be completed before flying resumes.
We will advise you depending upon your individual circumstances, with most people driving again only after both eyes have been treated.
When only one eye is being treated driving usually commences a few days after surgery.
Many people do not need to wear distance glasses after modern cataract surgery, but this is not guaranteed.
If there is clear distance vision, reading glasses are normally required unless there is a multifocal lens implant or monovision. For those with a multifocal implant or monovision, glasses may still be required for some tasks.
Further information on cataract surgery recovery can be found here.
This depends upon your occupation. Most people with office-based occupations resume work within a few days or a week.
Those who work in a dusty environment may need two to four weeks off work.
Most people make an excellent recovery and have good vision within a few days. It can, however, take up to six weeks for the eye to settle down fully.
Cataract surgery is usually an outpatient procedure, which means you don't have to stay in the hospital overnight. You'll be able to go home the same day as your surgery.
No. It is a same-day surgery that takes about 30 minutes for both eyes. You will be given a local anaesthetic to numb the eye, and you will be awake during the operation.
After the operation, you will spend a short time in the recovery area before being discharged home.
Cataract surgery is considered to be one of the safest operations.
Complications are rare, but the most common ones are infection, inflammation, bleeding and retinal detachment. Serious problems are rare, occurring in less than 1% of cases.
There is no difference in the quality of care between private and NHS hospitals.
The main difference is that you will be able to choose your surgeon and the type of IOL you want with private surgery.
With NHS surgery, you will be seen by the next available surgeon and will be offered a standard monofocal IOL.
If you choose to have private surgery, you will need to pay for the surgeon's fee, the cost of the IOL and the hospital's fee.
Private health insurance will usually cover the cost of cataract surgery, but you should check your policy to see if there are any exclusions.
During cataract surgery, your surgeon will place a special device into your eye to hold it open.
This can make some people feel anxious about blinking during surgery.
However, you will not be able to blink during surgery as the device will hold your eye open. If you do happen to blink, the device will prevent your eyelid from closing.
Book a FREE* Consultation
To get a better idea of how we can help you, and also the different types of services we offer, book a consultation now.

100% 20/20 vision
Focus Clinic has a remarkable 100% success rate for 20/20 vision. We know of no other clinic that has matched these results. There is a big difference between, for example, 98% and 100% success, especially if you are in the 2%.

10 year guarantee
Your 10 Year Guarantee means you can return at any time if you have additional questions on the quality of your vision. If you have distance vision correction for short-sight then any repeat laser eye treatments to correct a return of myopia in the first 10 years are included free of charge.*

Most trusted eye treatment clinic
We have the highest trust rating of any ‘eye treatment’ rated clinic, according to independent review site TrustPilot. With an outstanding 9.9 out of 10, when it comes to your eyes, choose the clinic that actual patients trust the most.