Book Your Free Consultation
Mr David Allamby
MD, FRCOphth, FRCS
WHAT ARE CATARACTS?
Cataracts are an eye condition that occurs when the normally clear lens of the eye becomes clouded. This can cause loss of vision, with sight becoming foggy or patchy, in turn restricting the sufferers’ level of sight.
‘What are Cataracts?’ – here at Focus, this is a question we get asked quite frequently. Throughout this article, I will look to provide you with an overview of not only what cataracts are, but how to spot the symptoms and the available treatment options.
Most common in people over 40, cataracts are the premier cause of blindness across the world. Unfortunately, the effects of cataracts cannot be removed with the use of glasses or contact lenses.

CHAPTER 1
There are three common types of cataracts that you may experience:
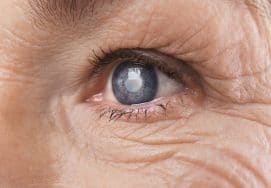
It is also possible to be born with cataracts already present in the lenses; this is referred to as a congenital cataract. Congenital cataracts can affect either one or both eyes simultaneously, severely hampering the visual development of newborns.
CHAPTER 2
Throughout our lifetime, proteins found within the eye may start to cluster together, causing clouding of the lens; this is the cataract. As we continue to age, this cloudy cataract portion is likely to spread throughout the lens, obstructing more of your vision.
Cataracts are most likely to develop throughout the ageing process, or if you have suffered an injury that affects the eye’s lens. Genetic defects may also play a part in your chances of developing cataracts.

While several risk factors have been identified, researchers are yet to definitively clarify the root cause for the development of cataracts.
Risk factors that contribute to the development of cataracts can include:
• Damage caused by excessive UV ray exposure
• Being overweight, especially obese
• Long term use of cholesterol medication
• Long term use of steroid medications
• Being very short-sighted
• Use of tobacco
• Steroid medications, particularly for a high dose or long-term use
• HRT (hormone replacement therapy)
• Alcohol abuse
• Historic eye injuries
• Any family history of the condition
• Old age
In most cases, cataracts will develop in both eyes, but not necessarily at the same rate, with one cataract potentially being more advanced than the other.
CHAPTER 3
During the early onset of cataracts, there will likely be little to no effect on your vision. But as the condition progresses, you will find your vision becoming slightly blurred or ‘foggy,’ like looking at the world through a pane of frosted glass.
You may also experience a higher level of photosensitivity (sensitivity to light) with indoor lights or the sun becoming very bright. When driving at night, this effect will become exponentially more noticeable, with headlights causing considerably more glare than before.

The exact symptoms you experience will vary on the type of cataract you are experiencing, and how developed it has become. During the early stages of nuclear cataract development, you may experience a much-improved level of near-sight vision; this is sometimes referred to as ‘second-sight’, caused by the hardening lens inducing a degree of short-sightedness.
This improved level of vision is only temporary and will fade as the cataract progresses. However, a subcapsular cataract may not present daytime symptoms until much later in its development but can lead to disabling glare at night, e.g. from car headlights.
If you find you are experiencing several of these symptoms I would suggest scheduling an appointment for an eye exam to confirm for sure you don’t have any of the following cataract symptoms:
• Blurry or dim vision
• Photosensitivity or glare from light sources
• ‘Halos’ around light sources
• Experiencing a yellowing of your vision
• Vision at night becoming increasingly worse
• Having double-vision within a single eye
CHAPTER 4
As it stands, researchers have yet to pinpoint the exact cause of cataracts but have identified several risk factors associated with their development. Because of this, doctors have made lifestyle recommendations to reduce the risk of developing cataracts, these include:
Let’s take a look at the different ways you can prevent cataracts from developing in the future:

Reduce exposure to UV radiation:
It is a good practice to prevent damage to your skin with the use of sun-lotion, but many people neglect to protect their eyes from harmful UV rays. Investing in a good UV rated pair of sunglasses, coupled with headwear featuring a wide brim will go a long way to reduce your risk of developing cataracts.
Watch Your Diet
Eating right should be a priority for all of us, but plays a more significant part in your eye health than many would expect. Those suffering from diabetes are at higher risk and will need to keep a keen eye on blood sugar levels. Fruits and vegetables high in antioxidants are ideal for maintaining eye health.
Reduce alcohol consumption
Evidence suggests drinking too much, or outright abusing alcohol, carries with it an increased chance of developing cataracts. Limiting alcohol consumption is good practice for all of us, but particularly those who have concerns regarding the health of their eyes.
• Quit smoking; while we cannot control any genetic predisposition we may have to developing cataracts, we can certainly take charge of our vices. Smoking is seriously damaging to our health overall, with ocular health being no exception. I would urge you to open discussions with your doctor about quitting, there are many strategies on offer from patches, to counselling that can help you curb your cravings.
• Regular eye exams; it is good practice to keep a routine that includes annual eye examinations, even if you feel that your vision is ok. Regular check-ups with eye care professionals will help to identify any early signs of cataracts, and a plethora of other eye-related disorders.
Hopefully, with developing research and technology, we will begin to understand eye health much more thoroughly than we currently do. As it stands, taking any of these points on board is sure to help maintain good vision and reduce the potential to develop degenerative eye problems.
CHAPTER 5
If you believe you are exhibiting symptoms related to cataracts, you will want to book in for an eye examination. During the exam, you will be asked questions regarding the symptoms you are experiencing, as well as perform several tests to allow the correct diagnosis to be made.
The three most likely tests/examinations that you will undertake to determine cataracts are:

1. Visual acuity test
At some point in your lifetime you will no doubt have already performed this test. A visual acuity test generally uses a white chart with a selection of letters featured on its face, with larger fonts at the top gradually becoming smaller further down the chart. You will be asked to read the letters from top to bottom, with a set distance between you and the chart, shielding one eye and reading with the other before swapping.
2. Retinal exam
Before beginning the retinal exam, your doctor will apply specially formulated drops to your eyes, with the intent of dilating (widening) your pupils. This will allow for your doctor to examine the back of your eyes (the retina), using a device known as an ophthalmoscope the lens can be checked for any signs of cataract.
3. Slit-lamp examination
you will undergo this examination so your doctor can inspect the front portion of your eye. Before beginning the exam, your doctor will apply specially formulated drops to your eyes, with the intent of dilating (widening) your pupils. This will allow your doctor to examine the entire lens as well as the back of your eyes (the retina), using a device known as an ophthalmoscope. A microscope equipped with a bright light which will be used to examine the cornea, iris and the lens of the eye directly behind it can be checked for any signs of cataract.
Following a cataract diagnosis, steps should be taken to reduce the impact cataracts can have on your daily life, but also to reduce the rate at which it may develop.
It is currently only possible to manage your symptoms, post-cataract diagnosis, without the need for surgery, but not eliminate them.
If you are diagnosed during the early steps of development, a stronger level of glasses prescription will provide you with an improved vision for a time. Some glasses can even help eliminate or reduce some of the glare you may be experiencing by featuring an anti-glare coating.
Using brighter lights for reading, preferably fitted with day-light bulbs, combined with new glasses or a magnifying glass, will allow you to continue reading for extended periods of time.
Once you start experiencing glare, or ‘halos’ around light sources, you should seek to limit any nighttime driving to only when necessary, for the safety of not only yourself but of other road users too.
Take a more invested approach in your own personal fitness, cutting down on smoking and alcohol, and following a diet rich in fruits and vegetables. This will not only improve your overall health but can help reduce the rate that cataracts will develop.
Unfortunately, whilst you can reduce the effect that symptoms of cataracts can have on you, with some lifestyle changes, surgery is currently the only effective treatment option available. Once your day to day activities become severely impacted, you should consider scheduling an appointment with your eye doctor to discuss your surgical options.
CHAPTER 6
Once cataracts are diagnosed, you will need to consider your next steps in terms of treatment. As surgery is the only treatment option currently available, a majority of doctors will suggest that a procedure will become necessary at the point cataracts begin to affect typical day to day tasks, such as driving or reading.
The decision should not be based on falling to a predetermined level of vision, e.g. worse than the driving standard, but on the impact it has on the patient’s life. Someone with cataracts may maintain 20/20 or better daytime vision but be disabled for night driving. If driving in the dark is necessary, this person should have surgery.
Since cataracts aren’t generally a painful condition, there is usually no urgent requirement to remove the cataract. However, cataracts will develop at a faster rate for people already dealing with diabetes.
Follow up eye examinations are recommended if you have opted not to receive surgery at this point, so your doctor can check on how the cataracts are developing over time.
If you do opt to receive cataract surgery, there is a number of different operations that may be used, depending on the type of cataract and how far it has developed. Each of these operations generally works in the same way, with the surgeon removing the clouded lens to be replaced with an artificial one.
While you may feel apprehension at the thought of having your eye operated on, these are routine outpatient procedures taking no more than 15 – 20 minutes. Although if cataracts are present in both eyes, they will need to be operated on separately, often one week apart, allowing the first eye time to heal.
Once all required examinations and discussions have been had with your doctor, they will decide on the best course of action to pursue. The method of surgery they choose to perform will most likely be one of three options:
Small-incision surgery (Phacoemulsification)
During small-incision surgery, also known as Phacoemulsification, a small ‘keyhole’ incision will be made in the cornea, allowing for a device to be placed in the eye emitting ultrasonic waves. These pulses will cause the cloudy lens to breakdown, allowing the tiny pieces to be removed before inserting the new artificial lens.
Large-incision surgery (Extracapsular cataract extraction)
This type of surgery is now much less common and is usually reserved for much more developed, larger, cases of cataract. The affected lens is removed in one piece before being replaced with the artificial lens. Recovery time will be expected to last slightly longer after this type of surgery.
Femtosecond laser surgery
Similar to small-incision surgery, femtosecond laser surgery instead makes use of a laser to break down the affected lens as well as creating the initial corneal incisions. Ultrasound will still be required but less energy is used as the initial fragmentation of the lens has been achieved by the laser. Again, after the lens has been broken down, an artificial lens will be put in place.
The results of femtosecond laser-assisted cataract surgery (FLACS) are no better than standard phacoemulsification, and may even have slightly higher complication rates. For this reason, FLACS has had limited uptake to date.
Usually, laser cataract surgery may be suggested for those who also suffer from more advanced cataracts.
CHAPTER 7
On the day of your surgery, it is common that your doctor may ask you to go nil-by-mouth (not consume any solid foods) for several hours before the operation. Before surgery you will receive either eye-drops or injections around the eye; this is a local anaesthetic, applied to numb any pain you could experience during the cataracts operation.
It is also possible to be given medication to help calm you during surgery as you will be awake throughout the procedure. Despite this, you will not be able to see what is happening to your eye as the surgeon works; instead, you will experience only general recognition of light and movement.
As with any surgery, there is an inherent risk of possible complications that you should be made aware of and consider, before deciding to undergo any procedure. Cataract complications include:
Possibility of infection
• Swelling to the front, or inside of the eye
• Detached retina (this occurs when the retina separates from the rear of the eye)
• Collateral damage to other areas of the eye
• Loss of vision
• The artificial lens may become dislodged
• Bleeding within the eye
• Chronic pain
It is also possible to develop what is known as PCO (posterior capsular opacification) after surgery, sometimes referred to as a secondary cataract. This is where your vision can become cloudy again; this can happen any time from as little as a few weeks post-surgery to developing years after surgery.
PCO occurs when the posterior capsule (this is where your original lens, and now your artificial lens is held in place) becomes cloudy after the eye has healed following surgery. If this does occur and you think you have developed PCO, you may need to undergo a simple 5-minute laser procedure called a posterior capsulotomy, sometimes called a YAG laser capsulotomy.
Cataracts Surgery Recovery – Time And Precautions
Cataract surgery is a quick and relatively straightforward procedure, meaning that recovery is also generally quick and straightforward. With most patients reporting improved vision after 48hrs with full recovery averaging around six weeks.
Immediately after surgery, your eyes will appear bruised and red; this is entirely normal and will subside within a few days. You will also be required to wait in the recovery area for around 30 minutes, to allow the sedation to wear off.
It is advisable to have someone drop you off and pick you up pre and post-surgery, as the local anaesthetic used can take several hours before it wears off.
24 Hours After Cataracts Surgery
For some people, clear vision will be present within just a couple of hours following surgery; however, each patient is different, and it could take up to a week or two for some people. It is possible for your vision to be distorted or cloudy, with some patients describing ‘wavy’ vision.
It is important not to panic, as your body is just adjusting to the new IOL that has replaced your natural lens, and these effects should subside over the next few days.
1 Week After Cataracts Surgery
During this period, your eyes may feel itchy, or gritty, and lights may appear very bright. Don’t be alarmed, this is normal.
Your vision should have seen a marked improvement compared to how it was immediately following surgery, with any bruising or redness starting to clear.
Within three to seven days you should be able to resume all normal activities, excluding swimming. Once you have met the DVLA standard, you will also be cleared to resume driving.
2-3 Weeks After Cataracts Surgery
Between 10 and 14 days, your eyes should have mostly healed. Around this point, you may need to be measured for new glasses, conditional on how well you have healed, and if your vision has stabilised.
This can come as a shock to some people; but regardless of the type of cataract surgery you have received, if monofocal implants have been used, you will likely require glasses for reading or computer use. The only exception is if you elected to have multifocal implants that restore vision over a range of distances.
1 Month After Cataracts Surgery
After four weeks you should have finished your course of eye drops. Any bruising or redness should be almost completely gone, with feelings of grittiness now in the past.
Vision will be remarkably improved compared to your experiences pre and post-surgery. If you hadn’t met DVLA standards for driving before you should do by now.
Swimming will also be allowed, provided you have double-checked with your surgeon, and he has given you the go-ahead.
I would recommend following these steps during cataract surgery recovery
• Avoid excessive touching or rubbing of eyes; eye-shields will be provided to wear while sleeping
• Avoid eye make-up
• Avoid any underwater activities
• Limit heavy lifting or strenuous exercise
• Keep soap and shampoo away from eyes
• Wear eye protection during windy days, protecting your eyes from grit and dust
It is important to note that it is unsafe to drive until your surgeon has checked your vision and approved you for driving again.
How Much Will My Vision Improve After Cataracts Surgery
Once the cataract surgery has been performed and the affected lens has been removed and replaced with a clear lens implant (intraocular lens, IOL), vision will be restored. For a majority of people, the results can be seen as soon as the next day, with many reporting better vision than ever before.
But there are several factors that will determine just how successful the procedure is for each individual:
• How developed the cataracts were before surgery
• Complications occurring during the procedure
• If you suffer from any other eye conditions, e.g glaucoma, diabetes or retinal problems
• The type of intraocular lens (IOL) used
• Healing time
I will take the time to expand a little more on each point raised, to give anyone considering cataract surgery an overview of the results that can be expected.
How Developed the Cataracts Were Before Surgery
The longer cataracts remain untreated, the further they will develop, meaning the end procedure could be more involved than if they had been removed in the earlier stages of development. If you wait too long cataracts can become hyper-mature, resulting in a loss of vision that will have a much greater impact on your day to day life.
Removing cataracts that have been left to mature increases the risk of surgical complications, due to the difficulty in removing the affected lens. This means you will be less likely to benefit from clear vision as a result.
Cataracts Surgery Complications
Adverse events or not common but could occur during the surgery and which might delay your recovery to clear vision. For example, the delicate capsular bag that envelopes the natural lens needs to be retained intact so that it can hold the new intraocular lens implant (IOL) in place. An inadvertent tear in this bag can lead to greater inflammation post-operatively and additional issues in inserting the IOL.
Suffering from Other Eye Conditions
If you already live with other eye conditions, it could affect the margins of how much your vision will improve post-surgery. Whilst it could increase the possibility of complications following surgery, the chances remain low.
If you suffer from high myopia (short-sightedness), the chance of retinal detachment following surgery is increased. Retinal detachment can be very serious and will require medical attention as soon as possible; the sooner treatment is administered the more likely it is for good vision to be restored.
Cataracts Surgery Lens Options
When it comes to picking an Intraocular Lens (IOL) to replace your cataract, there are 3 main types you can choose from. This can determine how much your vision could improve, how long it may take for consistent clear vision and whether or not you will require glasses.
• Monofocal lenses; these are the most common choice and usually used by the NHS. These will focus light onto just one point of vision, so you will require reading glasses after the operation. Toric monofocal IOLs can be used to correct astigmatism.
• Monofocal lenses with monovision; This is a good option if you would prefer not to be dependent on reading glasses. The surgeon performing the operation will adjust the power of one of your lens implants. This can be used to correct presbyopia (age-related long-sightedness) and reduce the need for reading glasses. However, it does require having cataract surgery on both eyes.
• Presbyopia-correcting IOLS; These premium lenses are the lens of choice if you suffer from presbyopia, most commonly available as trifocal lenses.
These implants are designed to improve reading and computer monitor range vision without having to compromise long-distance vision, and enhancing vision over a greater range of distances compared to monofocal options. However, not everyone’s eyes are suitable for these IOLs, and they are only available through private treatment.
Cataracts Surgery Healing Time
On average I would expect that you should have recovered anytime between four to six weeks after surgery.
However, it is difficult to pinpoint precisely how long this process takes from individual to individual, as every patient is different, and several factors can play a part in determining the timeline for a full recovery.
CHAPTER 8
The most significant factor in determining the success rate of cataract surgery is the condition of your eyes beforehand. This, unfortunately, is mostly out of your control but what is within your power is choosing the right clinic and surgeon for the job.
Lens Replacement Surgery Cost
Roughly 400,000 cataract procedures are performed in the UK each year, making it the most common operation of any speciality. Of course, it is reasonable to have reservations as the thought of eye surgery can be daunting for anyone.
Any good cataract surgeon or clinic will be open to discussion to alleviate any worries or fears you may have regarding the procedure.
There are several points to consider when you are considering cataract surgery:
• Experience; the more experienced a surgeon is, the higher the likelihood that they will be skilled at their job and deliver an excellent result
• Highly-rated surgeon and clinic; if a surgeon or clinic has a high number of excellent reviews, it is a sure sign they are leading the way in the delivery of cataract procedures. This can not only point to how adept they are in their technical capabilities but can be a key indicator in the level of customer service received throughout patient care.
• Excellent aftercare options; a lot of information can be extracted from a clinic’s customer reviews—a lot can be learned from the aftercare options on offer.
The best clinics will offer a wide variety to suit the differing needs of patients.
CHAPTER 9
Let’s take a look at the most common misconceptions about cataracts and a few surprising facts about them too!

Cataracts only affect the elderly; this is a common misconception held by a majority of people. Whilst true that most sufferers are advanced in age, cataracts can be developed at any point in a person’s life-cycle with newborns known to have been born with the condition.
• The development of cataract surgery dates back 2000 years. The earliest found references to cataract surgery date back to 29 AD, contained in De Medicina, authored by Aulus Cornelius Celsus. A copy of a written record of cataract surgery from the third or fourth century Egypt also points to the early origins of cataract surgery.
• Development of lenses used in cataract treatment arose during WWII; Sir Harold Ridley, while treating RAF pilots who had suffered eye injuries, discovered that when fragments of acrylic cockpit windows became embedded in the eyes of injured pilots, the body would not reject them, as would occur with glass. This observation led him to propose using artificial lenses in the treatment of cataracts; a technique still used to this day.
• Cataracts are the most significant cause of lost vision worldwide; the most likely demographic to develop cataracts is people over the age of 40. The WHO reports that 51% of all blindness worldwide is caused by cataracts, numbering roughly 20 million people, making it the leading cause of blindness worldwide.
• There is only one solution; while glasses and improved lighting may help alleviate the earlier symptoms of cataracts, this is not a final solution. Surgery remains the only effective treatment, involving the removal of the cloudy lens for it to be replaced with an artificial lens. As with any highly sensitive surgery, you must be sure to select the right clinic with an experienced surgeon.
• Reducing the risk; while there is no definitive way to prevent cataracts entirely, it is possible to reduce the possibility of developing cataracts. Adopting a healthy lifestyle, avoiding tobacco, and wearing sunglasses can all go a long way in reducing your chances of developing cataracts.
• Sun exposure can increase the chance of developing cataracts; it is well known that excessive exposure to UV rays can have a detrimental effect on skin health; the same is also true for your eyes. You can prevent ocular harm by wearing sunglasses rated for 100% UV protection
• Cataracts are painless; one of the main contributing factors to people not realising they have cataracts is because they develop painlessly, only becoming painful due to extreme sensitivity to light or acute attacks of glaucoma. Luckily, cataract surgery has developed to the point that procedures are now painless.
• The surgery takes between 10 – 15 minutes; cataracts are generally treated with a routine outpatient procedure under local anaesthesia, where the cataract-affected lens is removed and replaced with an artificial lens. Modern cataract surgery provides excellent results with advanced modern techniques utilising ultrasound and a keyhole approach providing an exceptional safety record.
Hopefully, this article will have gone some way to answering the question, ‘What are cataracts?’
If you are worried you may be showing symptoms of cataracts, or are experiencing problems with your vision and would like to book in for an appointment, we can be contacted here.
At Focus Clinic, our two on-site surgeons have a combined experience of over 45 years in the industry, and between them have performed over 35,000 procedures. Being one of the most experienced clinics in the UK, you can rest assured you will be left in safe hands.
Not only that but our exemplary customer service towards patients has us ranked at the #1 spot on Trustpilot, an independent review website for providers of eye treatment across the UK.
References:
https://www.ncbi.nlm.nih.gov/pubmed/20443769