Am I Suitable For Laser Eye Surgery?
The world of vision correction has come a long way over the years, and one of the most remarkable advancements in this field is laser eye surgery.
It has revolutionized the way we address common vision problems like nearsightedness, farsightedness, and astigmatism.
If you have been struggling with the inconveniences of glasses or contact lenses, laser treatment might be a life-changing solution for you.
But it's crucial to determine whether you are a suitable candidate for the procedure as there are a number of factors that need to be considered to ensure the best possible outcome.
Am I Suitable For Laser Eye Surgery?
If you meet the following criteria, you are 90% likely to be suitable for eye treatment, either with a laser procedure or possibly an artificial lens:
- Are you above 21 years of age?
- Has your prescription been stable over the last 12 months? (for distance vision; this does not apply to reading glasses)
- Can you see well with each eye when wearing glasses?
- Are your eyes healthy?
You will need a full consultation and eye examination to determine more accurately if you are eligible for laser eye or lens implant surgery.
Book your free telephone consultation today and a member of our team will be happy to talk you through the treatment options based on your individual circumstances.
Requirements For Laser Eye Surgery
We have been steadily increasing our knowledge about the characteristics of the ideal laser refractive surgery candidate since the first procedure was performed in 1988. We now have an extensive understanding of who is most suitable to undergo the procedure and, more importantly, who should be declined for treatment.
Understanding the ideal candidate characteristics can help patients understand whether treatment is an option for them and, if so, which procedure is most suitable.
Factors that affect laser eye surgery suitability are:
1. Age
There is no strict age limit for laser eye surgery, but age-related factors do impact eligibility. The minimum recommended age is generally 18, as vision can still change in younger people. As long as eye health and corneal condition are good, there is no upper age limit. However, after 55-60, some may prefer an implant-based option, such as refractive lens exchange (RLE), over laser eye surgery. The ideal candidate is over 18, as younger patients are more likely to have unstable prescriptions, which can make them unsuitable for procedures like LASIK or PRK.
Some patients over the age of 21 are still experiencing a high prescription, making them unsuitable for LASIK or PRK. Learn more about LASIK eligibility here.
However, it seems that the average age of candidates is increasing, and during recent years the mean age of subjects receiving surgery has shown an upward trend. This is likely due to how we use our eyes in the computer era, with increasing screen usage and less time outdoors. Both factors are linked to a progression in short-sightedness.
“The age of the patient is often linked to the type of treatment procedure that they will require.”
Younger patients in their 20s and 30s generally look to correct short-sight, with or without some degree of astigmatism. The usual choice of procedure is LASIK, with a minority of patients having PRK.
Middle-aged patients in their 40s and 50s often request treatment to assist with a loss of near vision. This is known as presbyopia and requires the use of reading glasses. This is usually treated using laser blended vision, though patients in their 50s are also candidates for refractive lens exchange (RLE).
Most commonly, patients aged 60 and over will require a refractive lens exchange (RLE), using a premium lens to correct both far and near vision. Cataracts (a whitening of the lens causing a drop in vision) become increasingly common after age 60. The surgery to remove them is identical to RLE.
Age Group | Comment | Procedure 1 | Procedure 2 |
|---|---|---|---|
18-21 | The prescription may not yet be stable | LASIK | PRK |
22-40 | Short-sight and astigmatism | LASIK | PRK |
41-49 | Developing presbyopia | LASIK for distance vision | LASIK Blended Vision |
50-64 | Established need for reading glasses | LASIK Blended Vision | Refractive Lens Exchange (RLE) |
65+ | Cataracts increasingly common | Refractive Lens Exchange (RLE) | Cataract surgery |
Table 1: Primary and secondary laser eye surgery and lens replacement options for various age groups
Is there a lower age limit?
The lower limit for treatment is 18. However, most patients with short-sight (the typical prescription in this age group) have not yet reached stability, and their myopia is often progressing. In practice, most patients are age 21 and over at the time of treatment.
Is there an upper age limit?
There is no official upper limit for laser eye treatment. However, cataracts become increasingly common after the age of 60, and the natural optics of the ageing lens inside tend to degrade over this age. A lens exchange procedure becomes the preferred choice for most patients in this age group.
2. Your Prescription
A patient's prescription should not have changed for one year before treatment. It can sometimes be difficult to definitively ascertain that this is the case, as the patient may not have visited for an eye examination for some time.
Myopia typically progresses for 10-15 years from the age of onset, and asking about the age of onset can be useful. Additionally, most patients have stabilised by their mid to late 20s.
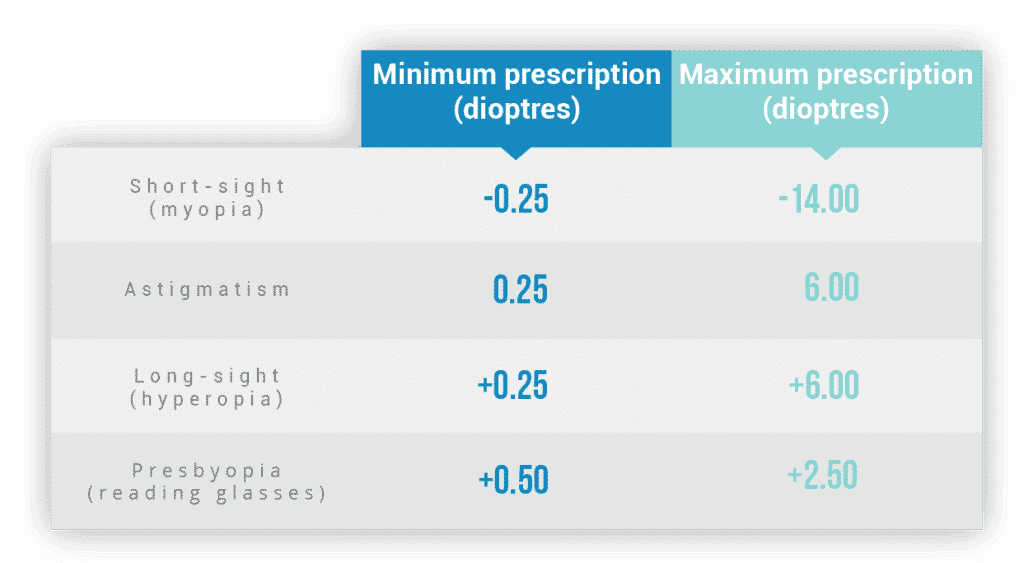
There are also minimum and maximum prescriptions that can be treated, so it's important patients fall within these ranges to be suitable for treatment. They are as follows:
3. Gender and Dry Eyes
Overall the number of men and women seeking vision correction is the same, with a consistent 50:50 split.
Both sexes show reluctance to wear glasses in certain situations. A recent poll showed that just over half of people took their glasses off when on a date or taking a selfie.
The main effect of gender is in the incidence of dry eye problems, which are more common in women.
A US study showed that dry eye disease (DED) affected 1 in 7 adults aged 48 or older, with approximately 50% more cases in women than men. Dry eye disease also affects postmenopausal women, those taking HRT or using the contraceptive pill.
Reliable epidemiological data from the large Women's Health Study and Physician's Health Study indicate the prevalence of dry eye leading to symptoms in the United States is about 7% for women and 4% for men over the age of 50, which equates to around 3.2 million women and 1.05 million men with DED in the United States.
Dry eye disease is a growing problem. Twenty-five per cent of patients who visit eye clinics report symptoms of dryness affecting their eyes, making it an increasing public health issue and one of the most common conditions seen by eye care clinicians. (Dry eye: diagnosis and current treatment strategies. O'Brien PD, Collum LM Curr Allergy Asthma Rep. 2004 Jul; 4(4):314-9.)
4. Type Of Refractive Error
One of the most important eligibility criteria for lens surgery is having stable refraction, which means that the prescription for glasses or contact lenses has stayed the same.
This usually occurs after the age of 18 to 22 years for short-sighted patients, with or without astigmatism. Patients are often asked to produce past refraction details from their optician visits for up to the previous three years to show that they have some stability.
A patient with a large recent change in refraction will be advised to wait until two consecutive prescriptions are similar. The goal is to avoid patients undergoing lens surgery and then finding that their prescriptions naturally became worse a year later, leaving them again with some degree of blur.
Laser vision correction for short-sight and astigmatism is typically very stable postoperatively and should last many years. However, if the eyes condition worsens and myopia progresses, it may incorrectly appear that the treatment has worn off.
Laser surgery changes the cornea's curvature and can correct most cases of myopia (short-sight), hyperopia (long-sight) and astigmatism. It can also correct the need for reading glasses for patients affected by presbyopia (the need for reading glasses in middle age).
Myopia is corrected by making the cornea flatter, while hyperopia is corrected by making the cornea more curved. In the case of astigmatism, the cornea is made more spherical.
The amount of refractive error with good outcomes has different ranges depending on the type of prescription and the excimer laser used. The table below shows the treatment range possible using the WaveLight Allegretto excimer platform:
Short-Sight Treatment Range
Short-sight between -0.25D to –14.00D is technically possible with the WaveLight platform, while other lasers have a lower range of correction. The limiting factor for extreme prescriptions is the thickness of the cornea, which will be measured at your consultation.
With the WaveLight system, which removes a smaller amount of tissue than some other lasers, most prescriptions up to -9.00 dioptres of myopia are treatable. Higher degrees of short-sight require a thicker than average cornea.
Astigmatism Treatment Range
Astigmatism can be corrected up to a severity of 6.00 dioptres. In the general population, 95% of astigmatism prescriptions are up to 2.00 dioptres, and most people have some degree of this refractive error, even if only minor, perhaps 0.25 or 0.50 dioptres. It is less common to have no astigmatism whatsoever.
Long-Sight Treatment Range
Although newer models of excimer laser platforms allow for larger ablation diameters, the predictability and stability of hyperopic refractive surgery continue to be lower than myopic corrections, especially at higher degrees of hyperopia.
Other potential challenges of hyperopic surgery include slower healing until the prescription is fully stable, fewer patients seeing 20/20 compared to short-sighted corrections, and higher retreatment rates.
These factors can reduce surgeons' willingness to perform hyperopic surgery. Most clinicians will not treat greater than +4.00 dioptres, even if the laser (as in the case of the WaveLight Allegretto) is approved up to +6.00.
If the patient is greater than 50 years of age, refractive lens exchange (RLE) may be a better option. RLE is a cataract operation in which the natural lens is removed and replaced with an artificial intraocular lens (IOL) of the patient's choice.
5. Personality
The motivation for treatment should be assessed carefully preoperatively, and patients should not feel coerced into the proceeding. Patients should have a cooling-off period between their consultation and treatment.
Expectations should be realistic, particularly when the prescription is very high or when treating long-sighted. Both these conditions may take longer to settle down than typical short-sighted corrections.
If the only acceptable outcome from your treatment is perfect vision, then you should appreciate that no medical intervention can guarantee a perfect result.
Laser vision correction produces a very high level of vision outcomes but cannot guarantee perfect vision for all patients. Perfectionists may not be good candidates for any laser eye treatment or lens-based surgery.
Patients with obsessive-compulsive traits or disorders may not be suitable for vision correction, as expectations can sometimes be unreasonably high.
Personality also plays a role in good aftercare. You will need to be of a mindset that understands the need for regular post-operative appointments and also be compliant in taking medications and eye drops when requested.
If you feel unable to attend regularly or use drops and tablets as instructed, you should not proceed with laser vision correction.
5. Tobacco Use
Cigarette smoking has been reported to be a factor in many clinical conditions that cause a dysfunctional tear film (the wet layer moistening the front of your eyes), resulting in dry eyes. A recent study has shown significantly poorer tear film stability and increased evaporation of tears in smokers.
Your tears are made up of a triple-layer sandwich. The innermost part is made from mucous, the 'filling' is the main watery layer (what we normally think of when we say 'tears'), and the outermost layer is a thin oily lipid layer produced by oil glands within your eyelids.
The oily layers act as a cling film, helping keep the water from evaporating too quickly. Your eyes are warm, and without the oil covering, tears would start to evaporate away in 2 or 3 seconds. With an effective oil layer in place, your tear film should be stable for 10 seconds or longer; that's plenty of time to keep your eyes wet until the next blink comes.
Smoking damages the ultra-thin fatty layer of the tear film, leading to excess evaporation. This can lead to many smokers having problems with dry eyes, including stinging or burning eyes and eye redness.
LASIK induces temporary dry eye for 3-6 months after treatment, and smoking can exacerbate symptomatic dry eye.
Because of the increased risks associated with smoking and LASIK, patients are advised to refrain from smoking for at least four to six weeks before surgery and then another four to six weeks after surgery.
Who Is Not Suitable For Laser Eye Surgery?
As a guide, patients in the following categories will generally not be considered for LASIK, PRK, or LASEK treatment, either for general health issues or previous eye problems.
- Auto-immune disease, e.g. rheumatoid arthritis, systemic lupus erythematosus—there may be an increased risk of inflammatory complications and possibly irregular healing.
- Patients with inflammatory bowel disease, e.g. Crohn's disease or colitis, have an increased risk of complications affecting the cornea.
- Immune suppression: conditions such as HIV or if the patient is taking immune-suppressing drugs (such as methotrexate, azathioprine, mercaptopurine) means an increased risk of infection or irregular healing.
- Pregnancy: during pregnancy and lactation, the refraction may vary, and there is an altered wound healing response. The patient must wait three months after giving birth or cessation breastfeeding.
- Oral steroids, e.g. prednisolone tablets—patients that have a condition requiring significant steroid use may also be at a higher risk of developing infections or other complications related to the state requiring steroid use.
- Roaccutane, isotretinoin: this drug causes a significantly decreased tear production. As above, the patient can be considered if the drug is stopped or substituted with the GP's consent for 3-6 months before treatment.
General Eye Health
Suitability for laser eye surgery is normally diminished if you suffer from:
- Severe dry eyes—patients with severe dry eyes should not have laser refractive surgery because the treatment can exacerbate the disease and make it extremely symptomatic. Patients with mild to moderate amounts of dryness may still be suitable with appropriate pre-treatment of the dry eye problems to meet the threshold required for safe laser eye surgery.
- Diabetic retinopathy—this is an absolute contra-indication as it can accelerate the progression of diabetic retinopathy. It has also been reported that pronounced aggravation of proliferative retinopathy has occurred after LASIK surgery. Diabetes that is well controlled and with healthy retinas may still be candidates for LASIK (but not PRK).
- Glaucoma—The optic disc is already compromised in eyes that suffer from glaucoma. During LASIK treatment, the intraocular pressure (IOP) is raised to above 90 mmHg, which may cause further damage to the optic disc. The topical steroids used postoperatively may also affect IOP management in these patients.
- Keratoconus and corneal disease—in dystrophies where the cornea is abnormally thin, the LASIK procedure would reduce the corneal thickness even more and may cause keratectasia. Signs of subclinical keratoconus, such as inferior steepening of the cornea beyond a certain degree, even where the corneal thickness is adequate, are a contraindication to LASIK.
- History of ocular inflammatory disease—eyes with recurrent inflammatory conditions, e.g. iritis or uveitis, will be more susceptible to an inflammatory attack after surgery which may be difficult to control. A prior occurrence of iritis that has not recurred and is not recent may not be a block to treatment. An experienced LASIK surgeon can advise based on your history.
- Herpetic ocular disease—there is evidence that corneal infection by herpes or zoster viruses can be reactivated by laser eye surgery.
- Sjögren's syndrome—these patients suffer from an auto-immune based dry mouth and dry eyes. LASIK or PRK/LASEK laser eye surgery will exacerbate their symptoms.
- Fuch's endothelial dystrophy—this condition affects the cell layer on the inside surface of the cornea, which is necessary to keep the cornea clear. In Fuch's dystrophy, the number of cells is reduced. While laser treatment has been shown not to affect the number of cells, the LASIK flap may not adhere well during the healing phase. PRK remains a possible treatment for such patients.
- Unstable refractive errors—the prescription must be fairly stable before treatment is considered. A change of more than 0.50 D equivalent in 12 months or less is deemed unstable.
- Visually significant cataract—in cases where there is a significant lens opacity indicating the development of a cataract (a whitening of the lens inside the eye), it is in the patient's best interest that this is treated first with cataract surgery. Further refractive surgery afterwards may or may not be necessary. Modern premium lens implants can be used to correct both distance and reading vision. Some patients over the age of 55 may opt for a refractive lens exchange (RLE) to correct vision instead of laser eye surgery.
- A squint or needing a prism that is not corrected by contact lenses.
- Blindness in one eye or partial sightedness—patients with significantly reduced vision of 20/40 or less in one or both eyes, e.g., optic nerve damage, macular degeneration, lazy eye, or other causes, should not have refractive surgery.
- Acute depression or obsessive-compulsive disorder (OCD)
- Difficulty in getting correct glasses—patients with many challenges finding a suitable glasses prescription may not be eligible for treatment due to the natural variation in healing that results from laser surgery. If a small residual prescription cannot be tolerated.
Conditions Requiring Assessment
Patients with the following conditions may be suitable for treatment, but it will depend on the individual's health and eye history. We have a guide that goes into more detail about laser eye surgery and medical conditions.
- Diabetes—LASIK may be suitable for people with diabetes who are well controlled and do not have signs of retinopathy (changes in the retina from the disease). PRK may lead to complications with healing and is not offered.
- Dry eyes—moderate dry eyes may be suitable for treatment with pre-treatment of any dryness. In patients with mild dry eye, it is unlikely to interfere with their eligibility. All patients should expect their eyes to be drier for 3-6 months after treatment, during which artificial tear drops will be used frequently.
- Blepharitis—is linked to dry eyes and should be pre-treated before surgery. There should be no infection present. The surgeon may expect the patient to adopt lid hygiene measures and, in some cases, use medication for several weeks before treatment.
- Epilepsy—the patient must remain relatively still during the LASIK or PRK procedure. Patients whose epilepsy is triggered by light may not be good candidates for treatment. Patients should not have had an epileptic episode for 12 months.
- Multiple sclerosis—will depend on the nature and progression of the condition.
- Increased internal eye pressure—eye pressure must be controlled before treatment, and there should be no evidence of visual field loss.
- Very large pupils with high correction—patients will be at higher risk of night vision symptoms after treatment and need appropriate counselling and advice.
- Very low prescriptions—if your prescription is very low and you do not normally wear correction, treatment may not necessarily be the right choice.
- Nystagmus—not all lasers have a tracker that can keep up with the involuntary eye movements associated with nystagmus.
Contraindications That May No Longer Apply
- Amiodarone—this drug was previously listed as a contraindication to have laser eye surgery. However, studies have suggested that amiodarone use may not increase the risk of having laser eye surgery or change the suitability for laser eye surgery. (Arch Soc Esp Oftalmol. 2016 Nov;91(11):520-525. doi: 10.1016/j.oftal.2016.05.005. Epub 2016 Jun 24.)
5-Hydroxytryptamine, e.g. sumatriptan—patients taking this drug were thought to have a higher risk of problems from the skin coating of the cornea. Research suggests this is not the case, and treatment may still be performed. (J Refract Surg. 2005 Jan-Feb;21(1):72-6.)
FAQs
To be eligible for laser eye surgery, you must be over the age of 18 and in good general health. You should not have any serious eye conditions, and your eyesight should be stable for at least two years.
There are some people who are not suitable for laser eye surgery. This includes people with certain medical conditions, such as autoimmune diseases, uncontrolled diabetes, or preexisting eye conditions. Breastfeeding and pregnant women are also not suitable for treatment.
Yes, a stable prescription is necessary for laser eye surgery. Your prescription should not have changed for at least one year prior to treatment. Laser eye surgery has specific minimum and maximum prescription requirements, so consultation with a qualified professional is essential to assess your eligibility for the procedure.
The cost of laser eye surgery in the UK can vary depending on a number of factors. These include the type of procedure you have, the clinic you go to, and whether you need both eyes treated. You can read more about the cost of laser eye surgery here.
Book a FREE* Consultation
To get a better idea of how we can help you, and also the different types of services we offer, book a consultation now.
Why Choose Us?

100% 20/20 vision
Focus Clinic has a remarkable 100% success rate for 20/20 vision. We know of no other clinic that has matched these results. There is a big difference between, for example, 98% and 100% success, especially if you are in the 2%.

10 year guarantee
Your 10 Year Guarantee means you can return at any time if you have additional questions on the quality of your vision. If you have distance vision correction for short-sight then any repeat laser eye treatments to correct a return of myopia in the first 10 years are included free of charge.*

Most trusted eye treatment clinic
We have the highest trust rating of any ‘eye treatment’ rated clinic, according to independent review site TrustPilot. With an outstanding 9.9 out of 10, when it comes to your eyes, choose the clinic that actual patients trust the most.
*Terms and conditions apply, excludes any age-related changes and conditions unrelated to the primary treatment
Customer Reviews