Glaucoma is something I discuss with patients almost every day. In fact, it’s one of the leading causes of blindness worldwide, damaging the eyes of 80 million people around the globe.
What is surprising is that half of the people living with it have no idea. That’s not because they’ve been careless. It’s because glaucoma is extraordinarily quiet in its early stages. It doesn’t announce itself with pain, blurred vision, or any obvious warning signs. It simply, silently, gradually takes your vision, often without you realising anything is wrong until significant damage has already been done.
What is Glaucoma?
Glaucoma is not a single disease. It’s a group of eye conditions that share one critical feature: progressive damage to the optic nerve, the highway that transmits everything you see from your eye to your brain.
In most cases, this optic nerve damage is driven by increased pressure inside the eye, known as intraocular pressure (IOP). Your eyes continuously produce a fluid called aqueous humour, which circulates and nourishes the internal structures of the eye before draining away through tiny channels.
At the heart of the eye’s drainage system is a structure called the trabecular meshwork. This is a sponge-like tissue that regulates how fluid drains. When the trabecular meshwork doesn’t function properly, the fluid can’t drain efficiently, it builds up, and the pressure inside the eye rises.
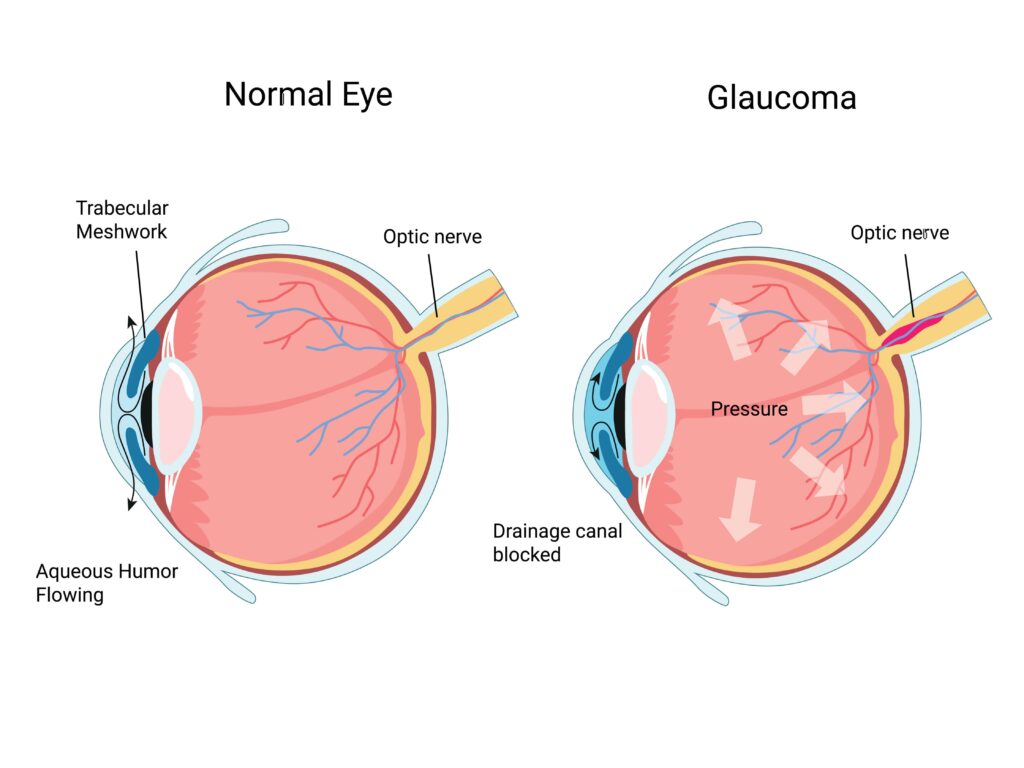
Over time, this elevated eye pressure puts the optic nerve under stress. And here’s the critical point: optic nerve fibres, once damaged, cannot regenerate. The vision they provided cannot be restored.
This is why glaucoma is classified as irreversible. But it is very often treatable when detected early. The goal is always to protect the vision you still have, and modern glaucoma treatment is very good at doing exactly that.
How common is Glaucoma?
Approximately 80 million people worldwide are currently living with glaucoma, and roughly half of them don’t know it. That figure is projected to rise to over 111 million by 2040 as the global population ages, making it one of the defining eye health challenges of our time. The Glaucoma Research Foundation describes it as a global epidemic.
In the UK, around 700,000 people are affected. Primary open-angle glaucoma, the most common form of glaucoma, affects roughly 2% of people over the age of 40, rising to approximately 10% of those over 75.
What causes Glaucoma?
The most common underlying cause is a drainage problem. When the eye’s drainage system becomes less efficient (due to age, genetics, or anatomy), fluid builds up, pressure inside the eye rises, steadily pushing on the optic nerve.
However, glaucoma isn’t purely a pressure problem. Some people develop optic nerve damage even with normal eye pressure. This is called normal tension glaucoma, and it’s a reminder that the nerve’s own vulnerability, its blood supply, and genetic factors all play a role alongside intraocular pressure (IOP).
Glaucoma is a condition in which multiple risk factors converge to place the optic nerve under strain. Pressure is usually the most significant and most controllable of those factors, which is why reducing it remains the cornerstone of treatment. We’ll explore how to treat glaucoma further in just a few moments, but first, let’s look at the different types of glaucoma.
The different types of Glaucoma
There are several types of glaucoma, each with distinct characteristics. Here are the four main ones:
Primary Open Angle Glaucoma
This is the most common type of glaucoma in the UK, and primary open-angle glaucoma (POAG) is what most people mean when they simply say “glaucoma.” In this form, the drainage angle inside the eye remains structurally open, but the drainage channels, particularly the trabecular meshwork, gradually lose their efficiency over time.
It develops slowly and is almost entirely painless. Most patients don’t notice any change to their vision for years, because open-angle glaucoma initially affects peripheral vision, which the brain is remarkably good at compensating for. By the time vision loss becomes noticeable, the disease has often already progressed considerably.
This type of glaucoma is frequently caught by an eye doctor during a routine comprehensive eye exam, long before the patient has any idea something is wrong. If you’re over 40, I’d encourage you to have regular eye checks to ensure it’s spotted in the early stages.
Angle Closure Glaucoma
Angle closure glaucoma is a very different beast. Here, the drainage angle of the eye becomes suddenly blocked, causing a rapid and dangerous spike in eye pressure. Acute angle closure glaucoma is a medical emergency, the kind of situation where hours genuinely matter.
The glaucoma symptoms of acute angle closure glaucoma come on quickly and can be severe: intense eye pain, headaches, nausea, vomiting, blurred vision, red eyes, and rainbow-coloured halos around lights. Some patients describe it as one of the most dramatic experiences of their lives.
If you or someone around you develops these symptoms, please seek urgent medical attention immediately. Do not wait.
Secondary Glaucoma
Secondary glaucoma develops as a consequence of another condition affecting the eye’s drainage system. Common causes include eye injury, internal eye inflammation (uveitis), prolonged use of steroid medications, advanced cataracts, or diabetes-related eye disease.
Pigmentary glaucoma is a specific subtype of secondary glaucoma that occurs when pigment granules shed from the iris block the trabecular meshwork and reduce drainage. Treatment for secondary glaucoma focuses on both reducing eye pressure and addressing the root cause.
Congenital Glaucoma
Congenital glaucoma is rare and occurs when babies are born with a defect in the eye’s drainage system. Signs can include enlarged eyes, excessive tearing, sensitivity to light, and cloudy corneas. Early diagnosis and surgical treatment of glaucoma are essential to protect the child’s vision.
Who is at greatest risk of Glaucoma?
While glaucoma can affect anyone, certain risk factors significantly increase the likelihood of developing it. Knowing your risk profile is the first step in protecting yourself.
Age
Age is the most consistent risk factor. The risk of developing glaucoma rises greatly after 40 and continues to increase with each decade. This doesn’t mean it’s inevitable, but it does mean you should be having your eyes checked regularly.
Family history
If a close relative has been diagnosed with glaucoma, your risk is four to nine times higher than average. If you have a family history of glaucoma, I’d recommend getting regular eye checks from an early age; don’t wait until you’re 40.
Ethnic background
People of African or Afro-Caribbean descent have a higher risk and earlier onset of primary open-angle glaucoma. People of East Asian descent have an increased risk of angle closure glaucoma. These differences are well-established and indicate that ethnicity is a genuine clinical consideration when assessing glaucoma risk.
Medical conditions and other factors
Several medical conditions are associated with a higher risk: diabetes, high blood pressure, significant short-sightedness (myopia), and long-sightedness (hyperopia) in those prone to angle closure. Corneal thickness also matters. Thinner corneas are associated with increased risk of glaucoma progression. Long-term use of corticosteroid medications is another known risk factor.
What are the symptoms of Glaucoma?
The honest answer is: in the early stages of open-angle glaucoma, usually none at all.
Primary open-angle glaucoma develops so slowly and so painlessly that most people don’t notice anything until peripheral vision has already been significantly eroded. Because the eyes compensate for each other, and because peripheral vision loss often begins subtly, blind spots can develop without the patient being remotely aware of them. By the time central vision is affected, the glaucoma symptoms people do notice, blurred vision, tunnel vision, and difficulty with contrast, often indicate that the disease is already quite advanced.
The warning signs of this type of glaucoma are often invisible to the person experiencing them, which is why routine eye examinations are so important. They ensure that glaucoma can be caught before irreversible damage occurs.
Acute angle closure glaucoma is the exception. It is anything but subtle. Sudden and severe eye pain, blurred vision, headache, nausea, and halos around lights are all characteristic. This is a medical emergency requiring immediate treatment to prevent rapid, permanent vision loss.
What does Glaucoma do to your vision?
Glaucoma typically begins by affecting peripheral vision, the edges of your visual field. As it progresses untreated, blind spots develop and gradually expand. The visual field narrows. Eventually, only central vision remains (what we call tunnel vision), and without intervention, even that can be lost.
The vision that is lost to glaucoma cannot be recovered. That is what makes early detection so critical. The damage cannot be reversed, but it can be stopped from going further.
Gradual vision loss due to glaucoma is one of the most preventable causes of blindness in the world. And yet it remains a leading cause of blindness globally, precisely because so many cases go undiagnosed or untreated.
How is Glaucoma diagnosed?
Glaucoma is most commonly detected during a routine dilated eye exam or comprehensive eye exam, often before the patient has noticed any change. Several tests are conducted to build a complete picture:
Eye pressure measurement (tonometry) checks the intraocular pressure inside the eye. Elevated eye pressure is a significant warning sign, though normal eye pressure doesn’t rule glaucoma out entirely.
Optic nerve examination allows direct visualisation of the optic nerve to look for characteristic signs of damage or structural change. An experienced ophthalmologist can often identify early features of glaucoma this way.
Optical Coherence Tomography (OCT) is a highly detailed imaging scan that produces cross-sectional images of the optic nerve and retinal nerve fibre layer. It can detect optic nerve damage at an extremely early stage, sometimes before any measurable visual field change. This technology has transformed how glaucoma is diagnosed and monitored in patients.
Visual field testing maps peripheral vision and reveals any blind spots that have developed. It’s also the primary tool for tracking whether the disease is progressing or stable over time.
A glaucoma diagnosis is typically based on the combination of these findings rather than any single test. That’s why a thorough assessment matters so much.
Glaucoma treatment options
There is currently no cure for glaucoma, but there are highly effective treatments, and the goal of all of them is the same: to reduce pressure inside the eye to a level that protects the optic nerve from further damage. To treat glaucoma successfully, the key is to start early and stay consistent.
Eye drops
Glaucoma medications, such as prescription eye drops, are the most common first-line treatment. Depending on the type, they either reduce fluid production in the eye or improve drainage. Many patients manage their glaucoma very successfully with eye drops alone, provided they use them consistently every day.
Laser treatment
Laser treatment, most commonly Selective Laser Trabeculoplasty (SLT), can improve drainage and lower eye pressure and is increasingly being offered earlier in the treatment pathway, sometimes as a first-line option rather than a last resort. Laser therapy is a straightforward outpatient procedure, generally well-tolerated, and can reduce or eliminate the need for daily eye drops in some patients.
In the UK, laser treatment for glaucoma is available on the NHS.
Surgery
Glaucoma surgery creates a new drainage pathway for fluid to leave the eye, reducing eye pressure. It has a longer recovery period than laser treatments and is typically reserved for patients with more advanced cases of glaucoma or where other treatments haven’t reached the desired outcome.
The right treatment plan is always an individual decision, based on the type of glaucoma, the degree of progression, and how the patient has responded to earlier treatment options. There is no single formula, which is why ongoing review with a specialist matters.
Can you live normally with Glaucoma?
In the vast majority of cases, yes, absolutely.
Most patients can continue to drive, work, travel, and live full, active lives. Glaucoma does not define or limit you, provided it is properly managed.
The patients who do best are those who engage with their care: who take their glaucoma medications consistently, who attend their follow-up appointments, and who understand that early treatment and regular monitoring are essential.
Can you have laser eye surgery if you have Glaucoma?
Refractive laser surgery procedures such as LASIK are not typically recommended for patients with glaucoma. These procedures temporarily increase pressure inside the eye during treatment, which carries additional risk when the optic nerve is already compromised.
That said, every case is different. Patients with very early or well-controlled glaucoma may still be candidates for certain procedures following a thorough assessment. If you’re considering laser eye surgery and would like to discuss your options, please get in touch with our clinical staff, who can advise you on the right course of action based on your eye health.
The importance of early detection and regular eye tests
If there is one message I want you to take from this guide, it is this: get your eyes tested regularly, and don’t wait until you notice something is wrong.
In the UK, adults are advised to have a full eye examination at least every two years. If you are over 40, have a family history of glaucoma, or have any of the risk factors described above, annual checks are well worth considering.
A comprehensive eye exam is quick, painless, and could prevent glaucoma from stealing your sight. Early detection means early treatment, and early treatment means the best possible chance of protecting your vision for the long term.
Ready To See Clearly?
Focus has a 100% 20/20 vision success rate for all common short-sighted prescriptions using it’s A-LASIK technique.

