Do you suffer (and that’s the right word!) with hay fever? Do you want to know more about what is going on, who’s the culprit affecting 90% of all those plagued by this seasonal nightmare and, more importantly, how you can gain some relief?
Yes, it’s that time of year when pollen allergies get us down with runny noses and red, itchy puffy eyes. Contact lenses become irritable, and laser eye surgery becomes an alternative means to be free from spectacles. But what is hay fever and why does it affect some than others? And what can you do to reduce the misery this year?
What Is Hay Fever?
Hay fever affects one in four Britons and costs the NHS almost 1 billion pounds per year. The disease was unknown 200 years ago. It was first described by a Liverpudlian-born London doctor called John Bostock who presented a case of a patient he called JB suffering from seasonal catarrh. The patient he described was, in fact, himself.
Allergic rhinitis, commonly known as hay fever, produces symptoms similar to that of the common cold. It usually occurs during the spring and summer months and is caused by an allergic response to pollens rather than a virus.
Pollen is a fine powder released by plants. It contains proteins, which can cause swelling, irritation and inflammation of not only the eyes but also of the nose, throat and sinuses.

Symptoms Of Hay Fever

Those who suffer from hay fever know these symptoms very well. Here’s a rundown of what is likely to torment you during the season when your particular pollen gets to work:
- Frequent sneezing
- Runny or blocked nose
- Itchy throat, mouth, nose and ears
- Itchy, puffy eyes
- Watering eyes
- Cough from mucus dripping down the throat (post-nasal drip)
Sufferers may also experience a loss of the sense of smell, known as anosmia, headaches, tiredness and facial pain from blocked sinuses.
Hay fever affects one in four Britons and costs the NHS almost 1 billion pounds per year.
There are approximately 30 types of pollens that produce hay fever. The most common type of hay fever, affecting around 90% of sufferers, is an allergy to grass pollen, which is at its peak level from mid-May to July each year. In the UK, 9 out of 10 hay fever sufferers are allergic to Timothy grass (Phleum pratense is an abundant perennial grass native to most of Europe) and Rye grass pollen (shown in the image below – Lolium is native to Europe, Asia and northern Africa, as well as cultivated in Australia and the Americas).
Tree pollens start earlier in the year, beginning in March and ending in June. Weed pollens usually follow on from grasses, running until September.
Pollen Seasons of Hay Fever
| Type of pollen | Season starts | Season ends |
| Tree pollen | late March | June |
| Grass pollen | mid May | July |
| Weed pollens | July | September |
Some people can also become allergic to spores released by fungi, which are most prominent in damp conditions. They can also grow indoors, e.g. underneath washing machines or sinks.
What Are The Risk Factors for Hay Fever

While the cause for the development of sensitivity to pollen is not fully understood, there are some factors which increase your likelihood of developing have fever:
- having asthma or other allergic condition, such as eczema (atopic syndrome)
- a family history of hay fever
- early childhood exposure to smoking (tobacco) and diesel exhaust particles
How does it affect the eyes?
An allergy occurs when the body’s immune system becomes more sensitive and reacts to an external factor in the environment. When an allergen comes into contact with the eye, antibodies attached to mast cells trigger the release of a chemical called histamine. This causes swelling and inflammation of the blood vessels and can cause them to leak.
Both eyes are usually affected and the symptoms tend to develop quickly. The white of the eye appears red and the eyelids become swollen. Patients usually complain of itchy, watery or scratchy eyes. Some patients may be sensitive to light and, in severe cases, patients may notice a fluctuation in their vision.
Hay fever eye symptoms
- Prominent itching of the eyes
- Watering eyes
- Scratchiness of foreign body feeling
- Swelling of the conjunctiva (can look like jelly)
- Light sensitivity
- Blurry, variable vision
When hay fever affects the eyes it is known as seasonal allergic conjunctivitis. The conjunctiva is the transparent mucous membrane that covers the white of the eye and lines the inside of the eyelids.
Conjunctivitis is usually due to an infection or irritation of the conjunctiva. In the instance of hay fever, it is due to an allergy and itching is a more prominent symptom.
Other Eye Allergies

Some patients tend to suffer from eye allergies year round which is known as perennial allergic conjunctivitis. It is a less common form of allergy but is usually caused by airborne particles such as dust mites, animal dander and fungus. These tend to be exacerbated in the autumn when exposure to these allergens is greatest.
A more severe eye allergy is vernal keratoconjunctivitis. This is more widely seen in patients who have eczema or asthma and primarily young men. Patients will complain of itching, watery eyes and thick mucous discharge. They may be sensitive to bright lights and notice a foreign body sensation.
Patients with a history of allergic dermatitis may have atopic keratoconjunctivitis. These patients tend to be older and male. The symptoms include severe itching and burning. The eye appears red and eyelids can be stuck together in the morning due to the production of a thick mucous.
Certain allergies, such as vernal keratoconjunctivitis and atopic keratoconjunctivitis, may require steroid eye drops so a visit to your eye specialist is advisable.
Contact lens wearers and some makeup, perfumes or other chemicals can also cause eye allergies.
When contact lenses affect the eye the eyelid can become swollen and cause giant papillary conjunctivitis. This is when large bumps form under the eyelid and patients complain of puffy eyes.
The cause can be due to an allergic reaction to a chemical in the contact lens solution, allergens such as pollen building up on the contact lens or a foreign body rubbing on the inside of the eyelid. If it is an acute response, such as a foreign body, there is usually an increase in excessive blinking and reflex tearing.

Management of Eye Allergies
OK, time to get you some help! Here are some top tips to reduce the suffering from hay fever:
- If you get any symptoms of eye irritation it is important not to rub the eyes as this can worsen the condition, leading to tiredness and puffiness of the eyelids and conjunctiva
- It is best to avoid using ocular irritants such as makeup and lotions
- Contact lenses should be avoided as they can exacerbate the symptoms, so it is advisable to leave them out until the symptoms have resolved
- Eyewashes can help with washing out foreign body particles such as dust, grit and smoke and eye drops can help soothe the symptoms. This can be particularly useful to aid children suffering from eye allergies.
- A cold compress can aid in reducing puffiness and calm inflammation. This can be done using either a flannel soaked in cold water or eye masks are now available to buy
- Trying to avoid the cause of the allergy may be difficult. On sunny days keeping windows closed, having air conditioning on and using wrap-around sunglasses when outside can help reduce the allergen. If all else fails, stay indoors when the pollen count is high
Eye Drops for Allergies
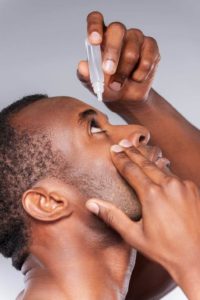
There are many drops available over the counter but it would be advisable to consult your optometrist first to direct you to the correct drops in line with your symptoms. Always read the label first and consult an eye specialist if you are aware of any pre-existing eye conditions.
- Eye brightener drops are readily available but they should only be used for a limited period for comfort and cosmesis.
- Artificial eye drops can provide temporary relief—there are many brands available and some have a higher viscosity which can make them last longer in the eyes.
- Mast cell stabilisers are the most common treatment option for eye allergies. Sodium cromoglycate is readily available over the counter without the need for a prescription.
- Combination anti-allergy eye drops, such as olopatadine, contain a combination of mast cell stabilisers and anti-histamine. They are available on prescription by your doctor.
- Antihistamine tablets can help with other symptoms of hay fever but tend not to be as effective with irritated eyes.
- In more serious cases, steroid eye drops may be required and can only be prescribed by an ophthalmologist. Steroid usage should be limited as long-term application can cause side-effects including glaucoma and cataracts.
Anti-allergy eye drops may take a week or so to have an effect before a noticed improvement. They need to be used regularly and continually for the entire period of the hay fever season.
If your symptoms are new, it would be advisable to have your eyes checked with your optometrist to diagnose the cause, as some more serious eyes diseases may share the same symptoms as allergies. Learn more about how eye allergies can affect children in our article.
Ready To See Clearly?
Focus has a 100% 20/20 vision success rate for all common short-sighted prescriptions using it’s A-LASIK technique.

